What’s the BIGGEST PROBLEM With Most Diagnoses?
… They’re Made TOO LATE.
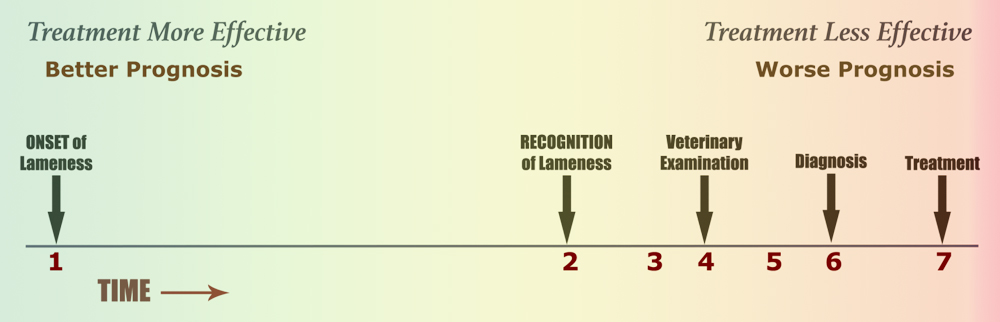
We currently rely on the horse owner or trainer (i.e. those that are best-situated to detect problems in their horses) to incite professional intervention. For instance, most of us equate the owner’s recognition of lameness with its onset. In reality, however, these events rarely occur at the same time.
Unfortunately, very few equestrians are trained in the skill of lameness recognition1 and accordingly may not detect problems unless they are chronic (long-standing) and/or severe in nature. In many cases lameness has been present for weeks, months or even years before it is acknowledged. The longer a problem persists, the more difficult it can be to treat. Eventual success often relies upon a speedy diagnosis.
- The onset of lameness. This represents the moment or period when the problem first occurs.
- Local recognition of lameness. This represents the moment when the primary caretaker (owner, trainer, barn manager, friend, farrier, etc.) discovers the existence of a problem.
- Veterinary notification of lameness. This represents the moment the veterinarian is first made aware of the problem.
- Clinical examination. This may be performed in the field or in a hospital setting. Physical assessment, passive and active soundness evaluations, palpation, flexion testing and local anesthesia (blocks) are common techniques implemented during the hands-on exam.
- Diagnostic imaging and testing. Radiography, ultrasonography, thermography, nuclear scintigraphy and magnetic resonance imaging (MRI) are imaging modalities commonly employed in modern work-ups of the lame horse. In some cases, clinical pathology (blood work) and histopathology (biopsy) are also performed to expedite a diagnosis.
- Diagnosis. The results of clinical examination, diagnostic imaging, and other testing often enable the veterinarian to reach a diagnosis, which represents the specific cause of the horse’s lameness.
- Treatment. Once a diagnosis is made, an appropriate treatment plan can be formulated. This represents a specific strategy used to return the horse to soundness. Corrective shoeing, systemic arthrotherapy (joint supplementation), local arthrotherapy (joint injections), extracorporeal shock wave therapy (ESWT), regenerative therapy (e.g. stem cells), chiropractics, etc. are strategies frequently employed in the treatment of equine lameness.
In order to help recognizing lameness at its onset, the equine professional has to:
- Regularly assess the horse in motion. Obviously, a professional can’t be in the physical presence of every horse every day. He or she can, however, visualize each horse on a regular basis through telemedical means. This modality is not as restricted by time, distance or money.
- Know what we’re looking at. GetSound® provides tutorials to help professional evaluators accurately interpret their visual impressions and make sense of what they see. Fortunately, there are a number of distinct visual markers that allow for accurate video assessment of the lame horse.2,3

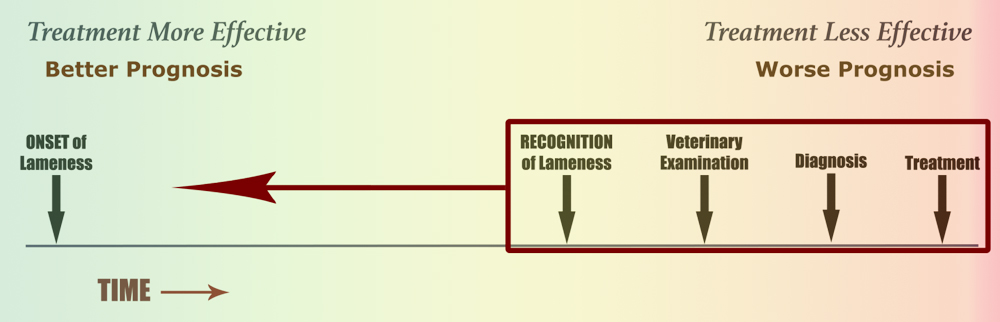
The key to successful management of our horses lies in our ability to proactively seek-out potential problems. Our intention is to detect problem during their “window of treatment opportunity”, aka the phase when treatment will be highly-effective. In other words, the goal of an effective management problem is to shorten the length of time between problem ONSET and problem RECOGNITION.
GetSound® telemedical review is a fast, easy and practical option built to help equestrians manage their equine partners.
- Greve L, Dyson S. The interrelationship of lameness, saddle slip and back shape in the general sports horse population. Equine Vet J 2014;46:687-694.
- Grisel GR. The use of remote digital motion analysis to assess equine lameness, in Proceedings. European Veterinary Conference Voorjaarsdagen 2013; 3-4.
- Grisel GR. Recognition and designation of specific gait signatures to aid in the digital assessment of equine lameness, in Proceedings. European Veterinary Conference Voorjaarsdagen 2013; 5.